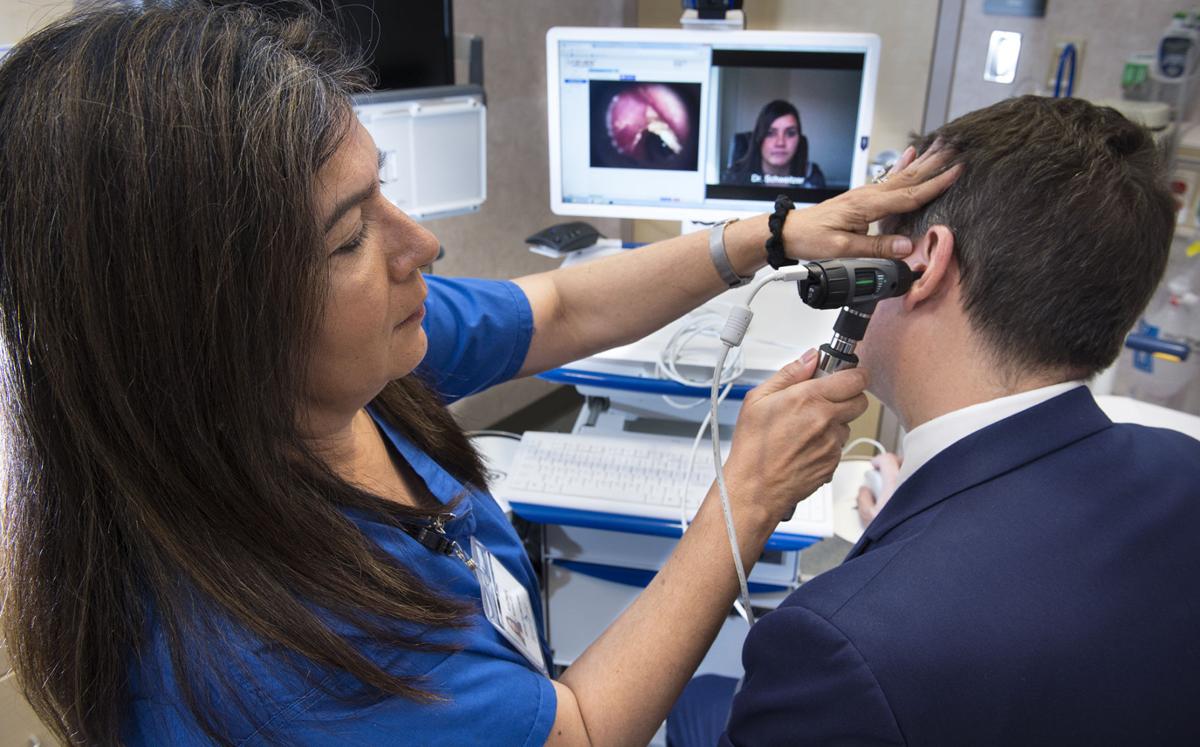
 With today’s digital technology, a doctor in Lincoln can examine a patient in the Panhandle and determine whether the patient needs to come to Lincoln for specialized care.
With today’s digital technology, a doctor in Lincoln can examine a patient in the Panhandle and determine whether the patient needs to come to Lincoln for specialized care.
That same doctor can look down a patient’s throat, in his or her ears, hear a heartbeat and determine whether immediate expert attention is needed — all via a computer cart equipped with diagnostic tools.
Through collaboration and technology, specialized health care is becoming available and convenient regardless of where a person lives in Nebraska.
It’s called telemedicine — or eMedicine — and it is transforming the health care system, giving patients access, attention and assessment at the touch of a screen, said Mandi Constantine, CHI Health’s division director of virtual services.
Want to publish your own articles on DistilINFO Publications?
Send us an email, we will get in touch with you.
In many cases, it is allowing aging or sick patients to stay in their own homes, rather than move to care centers or hire full-time health aides.
As technology advances and costs decrease, Constantine sees the future of more consumer-friendly and convenient quality health care.
In the past year, Bryan Health and CHI St. Elizabeth have introduced numerous e-services including virtual urgent care. Through it, people can, for a small fee, talk with health care professionals about their symptoms, send snapshots of their ailments, get diagnoses and, when needed, prescriptions without ever leaving home.
The hospitals have established similar partnerships with rural hospitals to provide diagnostic care and assessment in specialized areas including mental health, burns, prenatal, trauma and acute care. That means patients need not always travel for hours to receive follow-up treatment.
Virtual visits are beneficial to the patient as well as the physician, Constantine said.
In June, Bryan Health took virtual care a step further, providing eMedicine doctors based in Lincoln to be on call for long-distance, middle-of-the-night emergencies. Neligh’s Antelope Memorial Hospital was the first to go online, and more than 200 patients have been treated virtually over the past 10 months.
On March 10, Crete Area Medical Center went live and Lexington Regional Health Center is slated to start the program June 1.
Telemedicine is Nebraska’s answer to a growing shortage of rural health care providers, said Andy Whitney, director of Bryan Telemedicine Services.
“For local doctors it is quality-of-life issue,” he said. “They work in clinics during the day and cover the ER at night. It’s not a life doctors want. They don’t visualize a 24/7 life of being a doctor.”
Through Bryan’s eEmergency partnership, physicians assistants, nurse practitioners and doctors in Lincoln assess patients in Neligh or Crete through face-to-face interaction and a computer cart of diagnostic tools.
The eEmergency program remotely puts specialists in the room with hospital staff. For example, a mental health social worker has the benefit of visual cues when assessing a patient from afar and can determine whether that person needs to be admitted to Bryan’s mental health unit, or can be treated as an outpatient.
Nebraska has always been a leader in telemedicine, pioneering the use of video communications to deliver health care, according to a report by the National Institutes of Health.
In 1959, “Clinicians at the University of Nebraska used two-way interactive television to transmit neurological examinations and other information across campus to medical students,” the NIH wrote in his History of Telemedicine.
“They next explored its use for group therapy consultation, and in 1964 they established a telemedicine link with the Norfolk State Hospital (112 miles away) to provide speech therapy, neurological examinations, diagnosis of difficult psychiatric cases, case consultations, research seminars and education and training.”
Recognizing that telemedicine was an economical and practical way to get health care to rural areas and remote populations, the Nebraska Public Service Commission approved funding for the Nebraska Statewide TeleHealth Network in 2004.
The network is a collaboration of more than 110 sites including hospitals, health departments, mental health centers, physician offices and rural health clinics with the purpose of using video technology to extend health care resources to those in need particularly when it comes to specialized care such as radiology, endocrinology and mental health services.
The statewide network was created to provide rural facilities expanded services to save their patients the time, cost and inconvenience of traveling long distances for specialized care. In addition, it allows health care workers to receive training and education via video conference, as opposed to having to travel.
In 2011, the network provided 3,633 clinical consultations, according to an article published in Critical Care Nursing Quarterly.
“Among its many benefits, Telehealth increases access to specialty care for patients in rural areas; decreases travel time and saves money for patients and caretakers alike; provides the potential for earlier disease intervention; enhances clinical support between specialists and primary care providers; and serves as a medium for easy access to professional education, training and collaboration,” the report stated.
As technology becomes increasingly mobile, providers and patients can connect anywhere. From the convenience of their homes, patients relying on medical equipment can have information on the devices downloaded and sent directly to their doctors’ offices for evaluation.
And doctors can now receive vital medical on their smartphones.
“In a rural state dominated by Health Care Professional Shortage Areas and Medically Underserved Areas, Telehealth has the opportunity to help patients receive care at home,” the Critical Care Nursing article stated.
As long as technology improves, the possibilities for patients and physicians appear endless, said Whitney and Constantine.
This winter, Bryan worked with Lincoln-based Genesis Psychiatric Group to provide out-patient e-counseling using the hospital’s telemedicine video platform.
The service is available through Neligh’s Antelope Memorial Hospital, and will expand to Crete and eventually to Lexington, where other eMedicine
partnerships have been established.
When it comes to mental health, the partnership is huge, said Michelle Lemon, Genesis president.
In Nebraska, 48 of the state’s 93 counties have no mental health providers.
“Our goal is to make mental health services available to the vast underserved areas in Nebraska,” Lemon said.
Melissa Quick, a family psychiatric mental health nurse practitioner and Genesis’ telepsychiatry provider, has worked with hundreds of people.
“Nearly all of those that receive care via telemedicine are extremely satisfied with the service and individualized treatment,” she said.
St. Elizabeth, through its role with the Nebraska Telemedicine Network, provides virtual and remote monitoring of patients throughout Nebraska.
Last fall, St. Elizabeth piloted its Virtually Integrated Care program for CHI in Nebraska. The program offers telehealth services and monitoring to hospitalized patients.
Constantine compares the system to air traffic control. An experienced nurse sits behind a large console, monitoring vital signs for as many as 20 patients at a time. If a patient’s condition changes, that nurse can pull him or her up on video, talk to the patient and alert the team of nurses on the floor.
“It really gives the nursing staff another set of eyes and ears,” Constantine said.
And it gives patients quick access to a nurse who can answer questions, explain medical-speak and convey patient concerns to the hands-on staff providing care. That care team includes a registered nurse, licensed practical nurse and virtual tech.
Improved care at a cost-efficient price, said Libby Raetz, vice president of patient care services at CHI St. Elizabeth.
“It’s a second set of eyes,” said Raetz. “They can knock on the room door and have a conversation. They review vital signs and pain management and can interface directly with the team of three.”
St. Elizabeth started the program with eight beds last fall. Today, Virtually Integrated Care is available to 20 patients in the hospital’s medical/surgical unit. CHI is expanding the service to its hospitals in Kearney and Omaha.
“As health care dollar is shrinking we need to figure out ways to be more efficient and use our money more wisely,” Raetz said.
It allows health care professionals to keep up with increasing regulation without adding substantial cost. For example, state law requires that a pharmacist review all medication orders before being dispensed. Bryan’s ePharmacy program provides that review offsite for hospitals, so rural hospitals don’t need a pharmacist on duty 24/7.
Perhaps most important is that telemedicine allows patients and their families to be more in control, Constantine said.
“We are putting so many options in the hands of the consumer,” she said.
It also gives people the option to remain home. Bluetooth, sensors, videos and a host of apps have changed the elder care paradigm — homes can be made safe, and people can remain independent for longer.
“Telemedicine puts the consumer more in charge of their health,” Constantine said. “And that’s what we want. We want them to take charge of their health.”
Date: April 16, 2016









