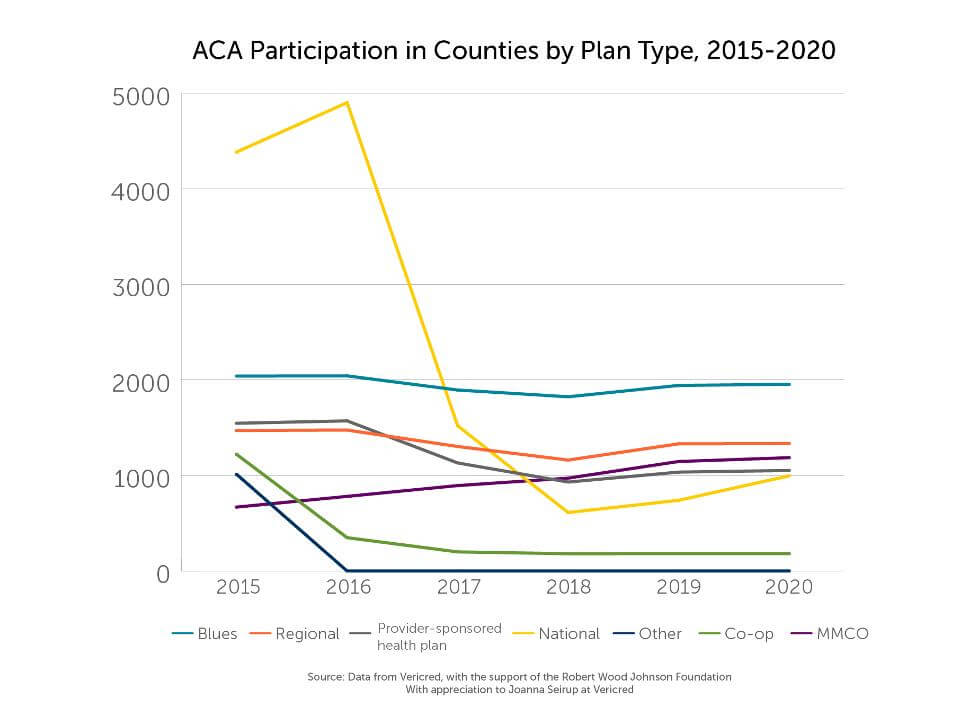
Aside from Anthem, Blue Cross and Blue Shield plans have been largely consistent in selling individual coverage under the Affordable Care Act for the last five years, according to a new market analysis tool from the Robert Wood Johnson Foundation.
In 2020, Blue Cross plans are projected to participate in 1,954 counties, which isn’t much different than the 2,040 counties where they offered individual coverage in 2015, the second year such health plans were offered under the health law, according to Robert Wood Johnson Foundation’s “ACA Market Participation Tracker.” The market tracker makes its debut before the seventh annual open enrollment period for Americans to choose health coverage under the ACA.
“The Blues have been the mainstay of the individual market, especially since the mass exodus of the national plans in 2017,” Kathy Hempstead, senior policy advisor at the Robert Wood Johnson Foundation, said in an interview. “Blues have been less likely to exit than other types of carriers.”
The Blues plans that have not exited tend to be nonprofit and owned by foundations or other tax-exempt entities, or like Health Care Service Corp., which is mutual and owned by policyholders. Health Care Service owns Blues plans in Illinois, Texas, Oklahoma, Montana and New Mexico.
“For one reason they have usually been able to absorb the loss, because they tend to be well capitalized,” Hempstead said of nonprofit and mutual Blues plans. “Another factor is that they have to make all their money in their state and they will create reputational damage by withdrawing, since they tend to be thought of as the carrier of last resort.”
Anthem, however, which operates Blues plans in 14 states, has scaled back its participation to a projected 555 counties for 2020. That compares to 911 in 2015. “Anthem has behaved much more like a commercial carrier than a Blue plan in terms of market participation, and has felt far more free to exit, creating some additional volatility in states like Missouri where Anthem carried the Blue license,” Hempstead said. Anthem is publicly traded and owned by investors.
Anthem said it is expanding next year and “will offer individual health plans for 2020 in select, additional regions of California and Virginia, as well as statewide in Connecticut,” the insurer said in a statement responding to data in the foundation’s ACA participation tracker.
“While it would be premature to comment about our participation in other markets where Anthem currently offers Individual health plans until regulators make this information public, Anthem’s approach to participate in the individual market remains disciplined and focused on those states that have demonstrated stability, which allow us to help ensure consumers have access to health plans that offer affordability and access to quality health care,” Anthem said.
Big national investor-owned and publicly-traded insurers including Aetna, a unit of CVS Health, Humana and UnitedHealth Group largely left the individual Obamacare market after being unable to successfully manage the costs of sick patients signing up for health coverage. That has left Blue Cross plans as the major provider of coverage as well as Centene, which has grown its Obamacare business gradually to nearly 2 million enrollees across 20 states, will be expanding again for 2020 and is the largest carrier of individual coverage on the ACA’s public exchanges. Centene is publicly-traded and poised to become a more national player should its proposed acquisition of WellCare Health Plans win regulatory approval in the next year.
Meanwhile, startups and smaller carriers including Oscar Health and Bright Health are making more money and have slowly grown their individual business under the ACA and are launching their biggest expansions for next year.
Cigna, which is a national carrier and last year bought the big pharmacy benefit manager Express Scripts, said Wednesday it was expanding offerings on the nation’s health care exchanges and in 2020 ACA-compliant plans will “be available in 19 markets across 10 states.”
Date: September 19, 2019
Source: Forbes