Plan ahead for the challenges of Robotic and Cognitive Process Automation
Healthcare has been a jobs engine but without improvement to health outcomes.
We are all aware of the constant increase in health care costs, with national health spending hitting $3 trillion in 2014. Higher costs are passed on to employers and patients with health premiums that exceed inflation. According to a recent HealthAffairs blog, industries in the rest of the economy shed millions of jobs between 2007 and 2009 in the severe recession. But not healthcare. Not only did healthcare workers increase by about 600,000 in these years, by January, 2017 there were 2.5 million more health jobs than at the start of the recession. This represents industry growth but with some disturbing trends. Between 1990-2012 about 95% of health industry job growth came from non-doctor workers that is now a ratio of 1:16. 10 of the 16 non-doctor workers are purely administrative and management staff, receptionists, information and office clerks. Such non-clinical labor is spread over the health systems, ambulatory care and payer segments. Most of these jobs are in revenue cycle management, claims processing, customer service and other related back office workers.
Healthcare administrative operations are bigger, definitely not better. According to the Institute of Medicine (IOM), the United States spends $361 billion annually on health care administration. The admin burden has become bloat that impacts productivity, profit and quality patient care.
Administrative complexities challenge every facet of the industry
How many of these administrative operations tasks and processes provide real value to the quality of patient care? There is no evidence that the increased complexity and spending has contributed to the improvement of care by any means.
Case in point: claims denial utilizing emerging technologiesOriginally denial management resulted in reworking and re-submitting for review of a technical denial, remonstrating with payers related to medical necessity, and making sure of reasonable expectation of payments. Due to margin pressures and efforts to increase reimbursements we kept adding processes. Now there are at least six different technologies and services used to manage denials, typically:
- Providing visibility to denial
- Denial analytics
- Real-time CDI improvement to reduce denials
- Denial collection services.
- Proactive and retroactive claims analytics
- Medical necessity review
Has this improved the reimbursements or reduced denials? Actually, no. We still have about 9% claim denial rate costing each hospital over $4.9 million a year which is 3.3% of net patient revenue. Total value of the claims denied is about $262 billion.
In 2010 David S. Wichmann, the current CEO of UnitedHealth Group, projected a savings opportunity of $332 billion in national health expenditures over the next decade. Based on the experiences within UnitedHealth, he observed that this could be achieved through the application of technology to administrative simplification. He made 12 key recommendations, most of which are still valid today. This shows how little progress we have made in using technology to simplify these processes.
Since that article we have seen compelling advances in healthcare management technology such as:
- Auto adjudication of claims
- Computer-aided coding
- Voice recognition for medical records
- EMRs that organize the clinical workflow
- EDI adoption
- Population health management analytics. and more.
Have these advances significantly reduced your administrative costs.? Instead of simplifying processes we seem to be compounding the complexities.
Outsourcing has not proven to be a panacea
Since 1990 the healthcare industry has also been at the forefront of organizations outsourcing jobs to low-cost locations such as India and Philippines. Between 1999 when I joined the industry, and now, there is a significant offshoring trend in revenue cycle management, claims processing and customer service. Even clinical jobs such as Nurse Calls are offshored.
Offshore outsourcing clearly reduces costs but managing these operations are adversely affected by inadequate capacity management, lower controls on quality, minimal investment in automation, reduced dependability, and the time and effort required to make changes in the operations.
“Servicing operations are too often treated as a Cinderella function – considered to be merely a cost center to be minimized, off-shored, or automated; or treated as the ‘problem child’ best outsourced to be someone else’s problem”.
– Richard Jeffery, Founder and CEO of ActiveOps, Experts in Back office Workforce Optimization
Does outsourcing as a cost containment tool truly deliver a competitive advantage for you? Experts in operations management have argued that the five elements in operations that are required to support competitive advantage of an enterprise are;
![]()
How do you rate for efficient back-office capabilities?
Many CEOs periodically demand cuts in back office operations. In a recent quarterly investor call (Q2, 2017) UnitedHealth group identified two key initiatives for the year. One of them was increasing efficiency and reducing costs in its services division – Optum. Optum provides back office services for UnitedHealth and other healthcare customers. One of the measures organizations resort to when cutting costs is “retrenchment,” often called re-organization. Barely four in ten companies meet their targets the first year in a cost-cutting program By year four fully 90% of back-office costs are back where they started. Sweeping cuts appear a fast and easy solution. But this can unintentionally lower business and process effectiveness. Risks of meeting service levels and customer commitments often lead to hiring back which negates the exercise and offers no long-term benefits.
Rather than “retrenchment,” focusing on improving operational efficiency drives sustainable cost reduction.
Real gains only come from having improved processes and having the control to deliver and sustain the benefits:
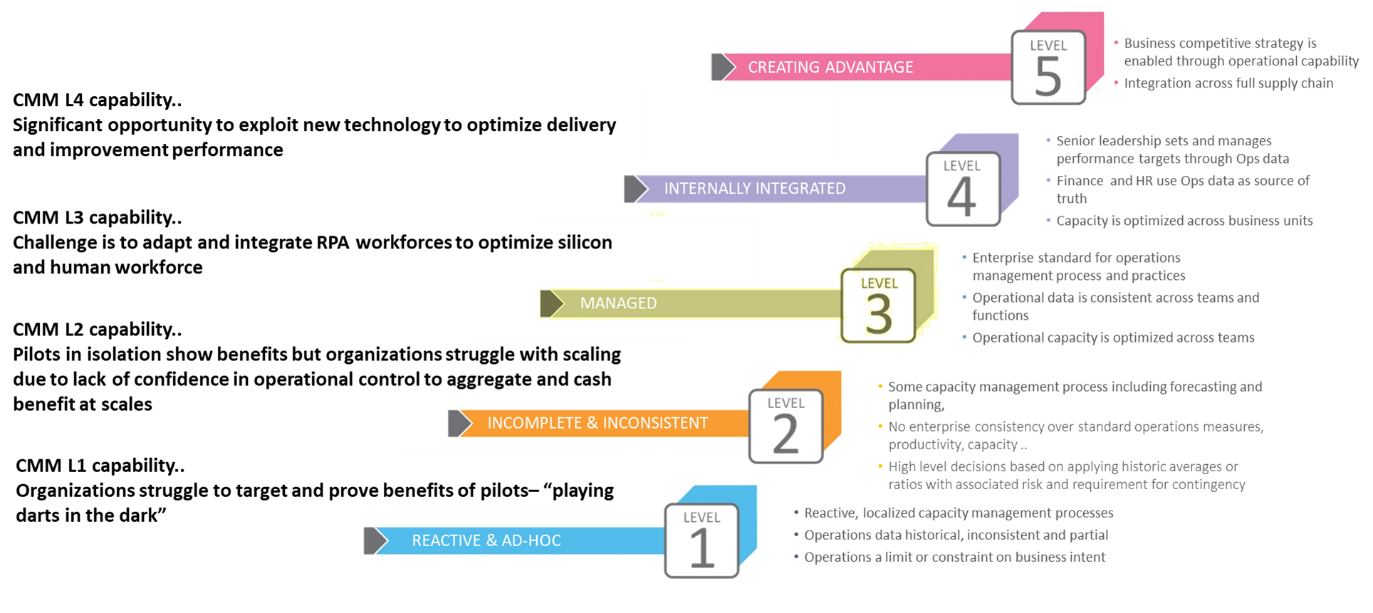
Most healthcare administration functions–revenue cycle management, claims processing and customer service are classified as Back Office. Investments in automation, RPA and other process improvements in these areas should be the catalyst for substantial cost reduction. All too often, however, perfectly valid improvements fail to deliver the expected benefit because of obsolete operations management practices which lack the precision and capability to “cash the check”. Using a Capability Maturity Model, ActiveOps provides an index of control effectiveness in back offices.
ActiveOps’ research across more than 550 “back office teams” of organizations worldwide found that the majority are languishing at Level 1 or 2. In fact, over 80% of the organizations were lower than Level 2, with very few approaching Level 5. What this means is most organizations lack company-wide standards or consistency for key operational metrics such as capacity, productivity and utilization. And so, they remain perplexed as to why they don’t see the gains they expected.
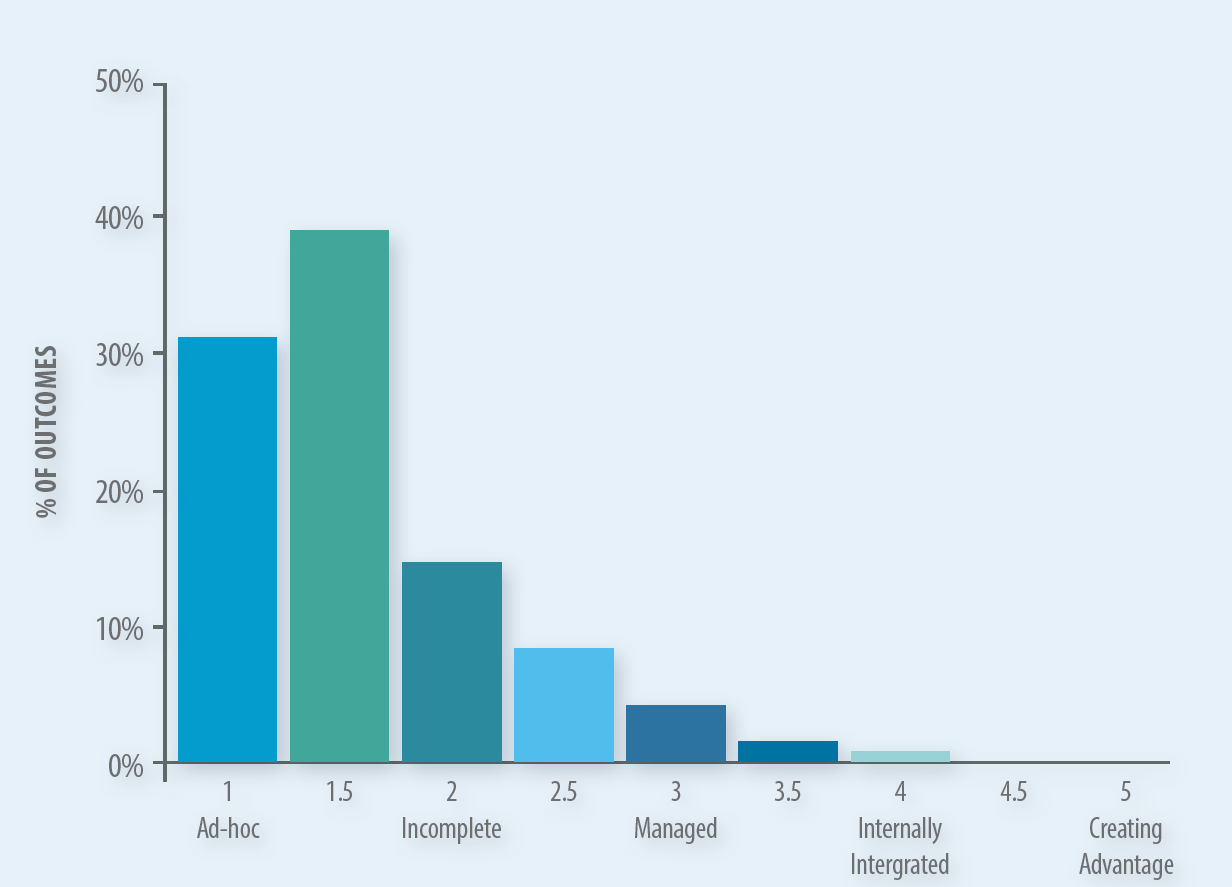
Figure 2: ActiveOps Capability Maturity Index – Source – ActiveOps Research of 550 back office teams, 2011-2016
Large providers such as UnitedHealth Group, Anthem and Humana have multiple back office operations in the U.S. and offshore. Adopting modern back office optimization methods would certainly be of great benefit to their efficiency and process optimization goals. Such methods provide transparency, reduce cost and waste (in some cases up to 25% has been demonstrated),before, and in addition to, improvements through automation or other process improvements. The net of both is then a huge step in efficiency and the associated cost and service gains for all stakeholders.
Approach Robotic Process Automation with the right strategy
There has been exceptional growth in the adoption of newer robotic and cognitive process automation (RPA and CPA) in the healthcare industry. These newer technologies can provide extraordinary speed, highly flexible capacity that result in increased accuracy in your back office operations. Some companies with extensive back office operations have been convinced of the value of RPA and are making significant investments in its deployment.
However, automating an already inefficient operation could be detrimental to achieving your objectives. One of the core prerequisites for implementing RPA should be a rigorous review of your existing operational efficiency levels. A careful and accurate assessment of your current capabilities and anticipated goals will optimize your investment, minimize risk, and attain the best possible value to your organization. Introducing RPA into an operation has profound effects on people and processes; identifying and managing all possible implications results in a successful implementation. Long-term planning with stages and milestones outweighs any focus on short-term performance increases. Considerations for an RPA implementation project include:
- What is our operational efficiency level – are we ready for automation?
- Are there any digital and process improvements need to be considered prior to implementing RPA?
- How will we measure and manage workforce optimization when process robots co-exist with human resources?
- Should Cognitive Process Automation be considered instead of RPA?
If yes, what are criteria and decision points?
By answering these questions, and others that arise in the assessment process, you will be able to make a positive business case for RPA.
The opportunities for process optimization and cost reduction
Administrative costs are steadily increasing, as well the use of as offshore outsourcing with all of its attendant flaws. Simplification of payer-provider interactions are critical to reducing inflated administrative operations that continue to have a detrimental impact on healthcare costs. Technology advances such as RPA, implemented correctly, will deliver effective cost containment and greatly enhance efficiency in healthcare administration tasks. Both providers and payers will benefit from these improvements in operational administrative efficiency. RPA adoption is gaining popularity as a powerful technology designed for operational process management. What results can you anticipate? An RPA-enhanced back-office operation can deliver a savings of 25-40% in terms of people and process optimization. The RPA application of process robotization combined with managed human resources can deliver unparalleled strategic value with long-term benefits. Starting with the right plan and knowledge base is an essential first step to maximizing RPA implementation success.
If you would like to explore the benefits of process optimization before embarking on RPA journey, please contact bmchittaranjan@cognitivehealthit.com
 BM Chittaranjan has over 20 years of experience with both start-ups and large enterprises, including global organizations. He is well-versed in people and process management having been responsible for the core operations and strategy for IT and business process operations (BPO) throughout his career. For the last 15 years he has implemented strategies for healthcare BPO and developed solutions for companies such as QSSI and UnitedHealth Group. Through this work he has achieved a keen acumen for technology evolution, cognitive design, and how to apply new technologies to business as his core competencies.
BM Chittaranjan has over 20 years of experience with both start-ups and large enterprises, including global organizations. He is well-versed in people and process management having been responsible for the core operations and strategy for IT and business process operations (BPO) throughout his career. For the last 15 years he has implemented strategies for healthcare BPO and developed solutions for companies such as QSSI and UnitedHealth Group. Through this work he has achieved a keen acumen for technology evolution, cognitive design, and how to apply new technologies to business as his core competencies.Date: Nov 07, 2017