To overcome the current challenges faced by the health system, a lot needs to change. First and foremost would be to build a strong pro-people non-commercialised public system as an alternative to the dominant for-profit sector
The global crisis, in the wake of the COVID-19 pandemic, has underscored the indispensability of a strong public healthcare system. As is the case with many other countries, in India too, the crisis exposed the weakness of the health system.
Due to systemic challenges that have perennially crippled the government health system, the response has been grossly inadequate. But the public sector and particularly the brave frontline health workers have been the only respite for people.
However, the role of private sector has been inadequate in overcoming the national crisis. Several news reports have exposed the regressive nature of the private sector. Either patients are being denied care, or charged high fees or being subjected to unnecessary tests to make money. There are also reports that patients’ families are being beaten up for non-payment.
Want to publish your own articles on DistilINFO Publications?
Send us an email, we will get in touch with you.
Here we would like to discuss some key features of private health care delivery in India, with an attempt to demystify some conceptions related to private health care delivery and point out some key concerns.
We would primarily use the two latest NSSO rounds Household Social Consumption: Health, the 71st (2014)[i], and 75th rounds (2017-18) and complement them with some other data sources.
Myth one: Private sector delivers care where government does not reach
The National Health Policy 2017 recognised private sector as an engine of growth. Several other policy pronouncements have been made with the understanding that the private sector complements government health services. Although the sector has grown significantly in the last three decades as an outcome of a series of reforms, much of this growth took place in metropolitan cities.
The government funded health insurance (GFHI) schemes, like the Prime Minister’s Jan Arogya Yojana (PMJAY), are fuelling further expansion of for-profit private hospitals through transfer of public resources to ensure a reasonable market in smaller towns.
At the outset, the plurality of the private health sector must be emphasised upon. The private sector is not a homogenous entity. It has both formal and informal providers as well as for profit and not for-profit entities under it.
The non-corporate private sector comprises of single doctor dispensaries, 2-10 bed nursing homes, medium-sized facilities. Additionally, India has the facilities of the recognised traditional systems of medicine. Meanwhile, the formal sector comprises large corporate hospitals, diagnostics chains, and stand-alone super specialty facilities.
There is hardly any comprehensive data available on the size and composition of the private sector. However, a census of health facilities in 63 major cities conducted in 2012 suggests that the distribution of private facilities favours metropolitan cities.
Distribution is most skewed in case of corporate hospitals as around 67 per cent of them are located in big cities. Some of the notable big cities include the four metros–Mumbai, Kolkata, Delhi, Chennai, and upcoming metros such as Ahmedabad, Bangalore and Pune.
Mumbai has shown the highest presence of health facilities among all the big cities. Out of 13,413 private facilities across all cities, Mumbai alone has 2,119 facilities – contributing to around 16 per cent.
As per the Periodic Labour Force survey (2017-18) data, out of every seven doctors only one is located in rural areas, rest of the six are located in urban areas.
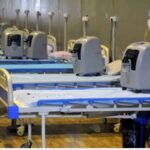
In the context of COVID-19, a key requirement for critical cases is the ICU beds. Approximately there were around 49 thousand ICU beds in private sector across all the cities. However, half of these beds are in 10 major cities, where the shortage of tertiary care facilities are less acute as many government medical colleges are located in these cities.
As per the 2012 data, there were more than 27 thousand ICU beds in public sector in these top ten cities. Thus, the private sector, rather than complementing the services of government, mushrooms around the tertiary government institutions to draw from the health care ecosystem created by public investment.
Another key feature of private hospitals is that most private facilities have less than 10 beds in their ICUs, which makes these places unviable for effective management of critical cases. Majority of the private sector outside these metro cities is much smaller in size, often equipped with five or less ICU beds. Rather than complementing public institutions, the private sector mushrooms around big government institutions.